Personalised Stratified Follow Up (PSFU)
There is currently little evidence that routine follow-up identifies disease recurrence yet it is costly and time consuming. Therefore national guidance encourages stratification of patients onto follow up pathways based on risk.
The NHS Operational and Planning Guidance places requirements on Cancer Alliances to roll out stratified follow up pathways for breast, colorectal, gynaecological and prostate pathways.
Patients should be stratified for follow up by their clinician following initial treatment based on clinical need. This ranges from professional led follow up for those to higher risk of disease recurrence to self management for low risk patients who following treatment will no longer have routine follow up appointments. Instead these patients are educated to self-manage their condition with back up from the clinical team and access to remote monitoring and re-entry pathways. A needs assessment is carried out and an individual care plan drawn up to address the needs of these individuals aimed at minimising risk and support to manage on-going conditions. .
The Cancer Alliance agreed a stratified follow-up pathway model can be seen below:
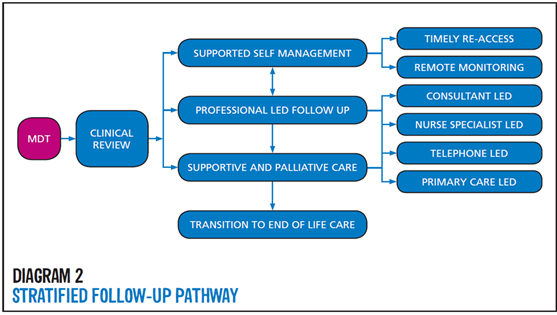
Gynaecology oncology stratified follow up clinical guidelines
The following guidelines have been developed in-line with national guidelines for stratified follow up and the treatment of patients with gynaecology cancer of ovarian or endometrial origin. This pathway is being offered to patients who meet the criteria by all Trusts across the Alliance.
Gynaecology oncology stratified follow up clinical guidelines
Breast Stratified Follow Up
In the North East and North Cumbria there are a number of Trusts who already offer this service, with the remainder working towards implementation by March 2019. The Cancer Alliance have approved a regional protocol based on one developed by nurses at Gateshead Trust.
Prostate
There is currently one Trust offering this service and another two looking to develop it. There are existing shared care agreements in place to enable patients to have monitoring undertaken in primary care so we are looking to build on this.
Prostate Stratified Follow Up Guidelines
Colorectal
The following stratified follow up guidelines have been revised by the Colorectal Pathway Group following their meeting in March 2024 for patients with colorectal cancer.
Colorectal Stratified Follow Up Guidelines
Head and Neck
The following stratified follow up guidelines have been developed by the Head and Neck Pathway Group for patients with head and neck cancer.
Head and Neck Stratified Follow Up Clinical Guidelines
Your Guide to Supported Self Management
The following booklet has been developed as a handy guide for patients, explaining what Supported Self Management is and addressing the most asked about concerns post treatment.